 | Antibodies Predict Development of Multiple Sclerosis |
 | Antibodies Predict Development of Multiple Sclerosis |
|
By Melissa Lee Phillips Neuroscience for Kids Consultant August 11, 2003
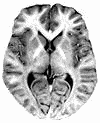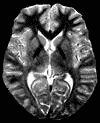
The neurologist performs a number of tests on you: she gives you a neurological exam, testing your senses, reflexes, and walking ability. She takes a magnetic resonance image (MRI) of your brain, and removes some cerebrospinal fluid for testing. When all the tests are in, she says that it's possible that you have multiple sclerosis (MS), but it's too soon to tell. You have many of the behavioral symptoms of MS. Your MRI shows that some of your myelin, the insulating fatty material that surrounds nerve fibers and allows them to conduct fast electrical pulses, has deteriorated. Your cerebrospinal fluid contains some antibodies -- proteins that your body makes to fight foreign molecules -- that are normally not found in healthy people, but are often seen in MS patients. The difficulty involved with diagnosing MS is a major frustration for patients and their physicians. Most of the symptoms seen in MS patients can be caused by other diseases. Many medications are available to treat MS, but because of unpleasant or even severe side effects, they usually are not prescribed. This diagnosis will not be given until the person has a second attack, and goes in for a second round of testing. The time between the first and second attacks is not only an uncertain and stressful time for the patient, but research suggests that this time period may represent an important window for starting treatment. Studies indicate that early treatment can lessen the immediate symptoms of an MS attack and minimize the long-term effects of the disease. The challenge, therefore, is for physicians to be able to diagnose MS earlier, so that treatment can begin earlier. Medical researchers at the University of Innsbruck in Austria recently made a discovery that could lead to an earlier diagnosis of MS. Thomas Berger and his colleagues (New England Journal of Medicine, July 10, 2003) reported that the presence of two antibodies in the blood serum of possible MS patients could predict if and when these people would develop clinically definite MS.
Berger studied 103 patients; all of these people had one initial neurological event that suggested they had MS. He took samples of their serum, the clear part of the blood left over when all cells and clotting proteins have been removed. He tested each patient's blood serum for antibodies to two different proteins: myelin basic protein (MBP) and myelin oligodendrocyte glycoprotein (MOG). Both of these proteins are components of myelin. In healthy people, the immune system recognizes that myelin is a component of the body itself, and so immune cells do not produce antibodies that attack myelin. In some people, however, this is not the case. Berger found that 22 of his patients had both of these myelin antibodies in their blood. Neither antibody was present in 39 patients, and 42 patients had antibodies to MOG, but not to MBP. The researchers' goal was to see if the presence or absence of these antibodies could predict if and when the patients had a second attack of MS symptoms. They found that it could: 95% of patients positive for both antibodies had a relapse, after an average of about seven months. Only 23% of patients with neither antibody had a second attack during the study, and if they did, it came at an average of almost four years later. The patients with only one antibody fell in between: 83% of them had a relapse, at an average of about one year later.
This is the first study to show a connection between these antibodies and the timing of an MS attack. Additional studies will be needed to confirm these results before doctors and counselors can begin to incorporate these findings in their patient care. But Berger and his coworkers believe that this work could be important for the care and counseling of people who might develop MS. Patients who have the antibodies in their blood would be counseled differently than those who don't. And, perhaps even more importantly, patients who are very likely to develop MS quickly might be placed on MS-regulating drugs sooner than patients who are less likely to develop the disease. This early treatment, many believe, could slow the disease enough to affect the long-term quality of life of people with MS. |
 Hear it! |
Antibodies | Autoimmune | Cerebrospinal Fluid |
| Demyelination | Multiple Sclerosis | Myelin |
| References and further information:
|
| BACK TO: | Neuroscience In the News | Neurological Disorders | Table of Contents |
![[email]](./gif/menue.gif) Send E-mail |
![[survey]](./gif/menusur.gif) Fill out survey |
![[newsletter]](./gif/menunew.gif) Get Newsletter |
![[search]](./gif/menusea.gif) Search Pages |