 |
Does Migraine Cause Brain Damage? |
 |
Does Migraine Cause Brain Damage? |
|
By Melissa Lee Phillips Neuroscience for Kids Consultant March 5, 2004
Migraine is a neurological disorder characterized by repeated, disabling
headaches. About a third of people with migraine also experience a
sensory disturbance called an aura, before or during headache
onset. These sensory symptoms are usually visual, such as flashing lights
or blind spots, but they can also be auditory. Previous research has
hinted at a possible association between migraine and brain lesions. In
this study, researchers, led by Mark C. Kruit, of Leiden University in the
Netherlands, examined Dutch adults. These people were divided into three
groups: those who had migraine with aura, those who had migraine without
aura, and a control group who had never suffered from migraine.
White matter lesions, which are often seen in people with Alzheimer's disease or multiple sclerosis, are usually more diffuse areas of cell death. Their underlying cause is not certain, although a decrease in blood flow has been implicated. White matter lesions involve only neuron axons; infarcts also destroy cell bodies. The researchers found that more people with migraine than without migraine had infarcts in their brains. But this result was not statistically significant -- that is, the higher rate of infarcts in the migraine group could have been simply a coincidence.
When Kruit and his team inspected diffuse white matter lesions in the brains of their subjects, they found a significant correlation with migraine only in women, and only if the lesions were in the periventricular area of the brain, right around the ventricles. For these people, the increased frequency of migraine attacks was associated with more white matter lesions, just as it was with infarcts in the PCT. |
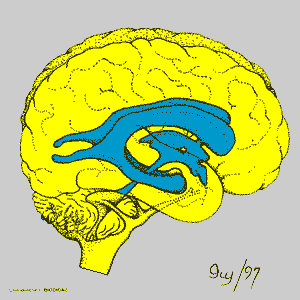 The fluid-filled ventricles in the middle of the brain. (Image adapted from Biodidac) |
The researchers speculate that the trauma the brain experiences during migraine attacks is directly killing brain tissue, although they acknowledge that there could be a third, unseen factor contributing to both migraine and brain lesion development. In the past, physicians have generally viewed migraine as an episodic disorder--patients experienced attacks from time to time, but they didn't seem to be getting any worse. This study, in conjunction with previous work, indicates that, at least for some people, migraine is progressive: more attacks mean more brain damage. And although not all migraine patients appear to be at risk, some may experience not only debilitating pain and visual disturbances, but also the decay of small parts of their brains. |
|
For references and more information, see:
|
| GO TO: | Neuroscience In The News | Explore the Nervous System | Table of Contents |
![[email]](./gif/menue.gif) Send E-mail |
 Get Newsletter |
 Search Pages |