 | A Glimmer of Hope for Huntington's Disease Patients |  |
 | A Glimmer of Hope for Huntington's Disease Patients |  |
| By Ellen Kuwana Neuroscience for Kids Staff Writer January 11, 2001
Basic Facts about Huntington's DiseaseResults from two research groups provide hope to the people who battle against Huntington's disease (HD). HD is a relatively rare disease, affecting approximately 30,000 people in the US. HD is an inherited neurological disorder: if either parent has it, his or her child has a 50-50 chance of getting it. Symptoms, which usually appear after age 30, include dementia, chorea (jerky, random movements of the body), poor coordination, depression, memory loss and mood swings. Although there are a few drugs that help with the symptoms, there is no treatment for HD and patients often die within 15 years of the onset of symptoms.
Inside the HD Brain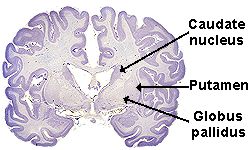 HD damages neurons in the area of the brain called the basal
ganglia, especially the caudate nucleus and globus pallidus. What if there
was a way to replace these damaged brain cells? Using rodent and primate
models of Huntington's disease, researchers have taken fetal brain cells,
transplanted them into brains damaged by HD, and shown that the
transplanted cells survive. Would this technique work in humans and if the
cells survived, would they do the jobs that the damaged cells previously
did such as form connections, relay signals, and secrete
neurotransmitters? HD damages neurons in the area of the brain called the basal
ganglia, especially the caudate nucleus and globus pallidus. What if there
was a way to replace these damaged brain cells? Using rodent and primate
models of Huntington's disease, researchers have taken fetal brain cells,
transplanted them into brains damaged by HD, and shown that the
transplanted cells survive. Would this technique work in humans and if the
cells survived, would they do the jobs that the damaged cells previously
did such as form connections, relay signals, and secrete
neurotransmitters?
First Time Transplanted Fetal Cells Survive and Improve HD Symptoms in HumansMarc Peschanski and colleagues harvested fetal neurons from the area that was destined to develop into the striatum and transplanted these cells into the striatum of adult patients with mild to moderate HD. These patients had exhibited symptoms of HD for two to seven years. The scientists then evaluated the patients one year later with magnetic resonance imaging (MRI) and positron emission tomography (PET) scanning techniques to "see" how the brain was functioning. The results from five HD patients (experimental group) were compared to 22 untreated patients (control group). Although these results are encouraging, it is difficult to draw conclusions from this study because of the small number of study participants: only five people underwent the transplantation. It is also difficult to compare the experimental and control groups, as HD symptoms vary considerably. To address these issues, the researchers are planning a clinical trial involving 60 patients in France and Belgium.
Transplanted Fetal Cells Survive, Form Connections and Remain Disease-FreeIn another similar study led by Dr. Thomas Freeman and Dr. Francesca Cicchetti, fetal striatal neurons were transplanted into the striatum of adult HD patients. For the first time, it was shown that these grafts (transplanted cells) can survive and develop in the adult brain. Furthermore, the transplanted cells did not degenerate, meaning they were unaffected by the disease process.
Outlook for Fetal Tissue TransplantationIn related research, fetal tissue transplants have been shown to improve symptoms of Parkinson's disease. However, this approach may be more challenging in Huntington's patients because the disease affects more of the brain. Furthermore, drug therapies may be cheaper and easier to administer to many people. Additional studies are needed to assess how feasible fetal cell transplantation will be as a treatment for HD. Nevertheless, this research is one step closer toward finding a cure for Huntington's disease. |
Did you know? | Folk singer Woody Guthrie (1912-1967) had Huntington's Disease. He inherited the disease from his mother, who died of HD when Woody was 15 years old. Two of Woody's children also had HD, although his singer-songwriter son, Arlo Guthrie, has apparently been spared. |
|
References and further information:
|
| BACK TO: | Neuroscience In The News | Table of Contents |
![[email]](./gif/menue.gif) Send E-mail | ![[newsletter]](./gif/menunew.gif) Get Newsletter | ![[search]](./gif/menusea.gif) Search Pages |  Donate to Neuroscience for Kids |