Exciting the Immune System to Fight Amyloid Plaques
 The
researchers took advantage of the immune system's defense properties
and taught it to recognize beta amyloid as an unwanted invader. This is
like teaching a guard dog a new trick. They created a "vaccine" that
combined beta amyloid with a substance that mobilizes the immune system.
This vaccine caused the immune system to mount an attack against beta
amyloid, which in turn reduced the number of plaques in the brain. (It's
as if you were baking cakes and someone took away some of your batter.
You wouldn't be able to bake as many cakes and each cake would
not be as big.) The
researchers took advantage of the immune system's defense properties
and taught it to recognize beta amyloid as an unwanted invader. This is
like teaching a guard dog a new trick. They created a "vaccine" that
combined beta amyloid with a substance that mobilizes the immune system.
This vaccine caused the immune system to mount an attack against beta
amyloid, which in turn reduced the number of plaques in the brain. (It's
as if you were baking cakes and someone took away some of your batter.
You wouldn't be able to bake as many cakes and each cake would
not be as big.)
What is truly exciting about the results from this study is that the
vaccine not only prevented further plaque formation, but it reduced the
amount of existing plaques!
Testing the Vaccine, Experiment #1
 How did the scientists test the vaccine? In a good experiment,
there is a control group and an
experimental
group. The control group serves as a comparison for what happens
in the experimental group. The experimental group receives a new
treatment, whereas the control group does not. The two groups are
treated identically in all other ways.
How did the scientists test the vaccine? In a good experiment,
there is a control group and an
experimental
group. The control group serves as a comparison for what happens
in the experimental group. The experimental group receives a new
treatment, whereas the control group does not. The two groups are
treated identically in all other ways.
In the AD vaccine experiment, young mice (6 weeks old) were genetically
engineered to produce lots of amyloid protein, more than normal mice would
produce. Mice at this age have very few brain changes, such as plaques
formation, associated with AD.
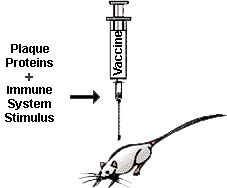
The experimental group received the "vaccine" of beta amyloid plus an
immune system stimulator. The control group received everything except the
beta amyloid. For 11 months, each group received one injection per month.
When the scientists examined the mice brains, the control group had
plaques covering 2-6% of their brains, while the group who received the
"vaccine" had very few plaques. So the vaccine "essentially prevented the
development of beta amyloid plaque formation," the report in Nature
states. What's more, beta amyloid production was unaffected. This means
that either the protein was being prevented from clumping into plaques, or
it was being cleared out of the brain more effectively. |


 The
researchers took advantage of the immune system's defense properties
and taught it to recognize beta amyloid as an unwanted invader. This is
like teaching a guard dog a new trick. They created a "vaccine" that
combined beta amyloid with a substance that mobilizes the immune system.
This vaccine caused the immune system to mount an attack against beta
amyloid, which in turn reduced the number of plaques in the brain. (It's
as if you were baking cakes and someone took away some of your batter.
You wouldn't be able to bake as many cakes and each cake would
not be as big.)
The
researchers took advantage of the immune system's defense properties
and taught it to recognize beta amyloid as an unwanted invader. This is
like teaching a guard dog a new trick. They created a "vaccine" that
combined beta amyloid with a substance that mobilizes the immune system.
This vaccine caused the immune system to mount an attack against beta
amyloid, which in turn reduced the number of plaques in the brain. (It's
as if you were baking cakes and someone took away some of your batter.
You wouldn't be able to bake as many cakes and each cake would
not be as big.) How did the scientists test the vaccine? In a good experiment,
there is a control group and an
experimental
group. The control group serves as a comparison for what happens
in the experimental group. The experimental group receives a new
treatment, whereas the control group does not. The two groups are
treated identically in all other ways.
How did the scientists test the vaccine? In a good experiment,
there is a control group and an
experimental
group. The control group serves as a comparison for what happens
in the experimental group. The experimental group receives a new
treatment, whereas the control group does not. The two groups are
treated identically in all other ways.  For this experiment, researchers used mice who were old enough to have
developed plaques (11 months old). Again, each mouse got an injection
(either of vaccine or just the immune stimulator) once a month. Half of
the mice from each group were examined after four months of treatment (15
months) and the other half after seven months of treatment (18 months).
The results here were surprising and stunning. The control group had a
17-fold increase in plaques! The experimental group, the mice who had
received the "vaccine," not only developed fewer plaques, but what plaques
they had at 11 months were reduced at the 18-month
point! This means that not only did the vaccine prevent further plaque
formation, it reduced existing plaques, too! Because the goal of the
vaccine
was to decrease the amount of beta amyloid in the brain (and the numbers
of plaques), the lower numbers here show that fewer plaques were seen in
the brain. The vaccine appeared to have worked!
For this experiment, researchers used mice who were old enough to have
developed plaques (11 months old). Again, each mouse got an injection
(either of vaccine or just the immune stimulator) once a month. Half of
the mice from each group were examined after four months of treatment (15
months) and the other half after seven months of treatment (18 months).
The results here were surprising and stunning. The control group had a
17-fold increase in plaques! The experimental group, the mice who had
received the "vaccine," not only developed fewer plaques, but what plaques
they had at 11 months were reduced at the 18-month
point! This means that not only did the vaccine prevent further plaque
formation, it reduced existing plaques, too! Because the goal of the
vaccine
was to decrease the amount of beta amyloid in the brain (and the numbers
of plaques), the lower numbers here show that fewer plaques were seen in
the brain. The vaccine appeared to have worked!

![[email]](./gif/menue.gif)
![[survey]](./gif/menusur.gif)
![[newsletter]](./gif/menunew.gif)
![[search]](./gif/menusea.gif)
![[notes]](./gif/menunot.gif)